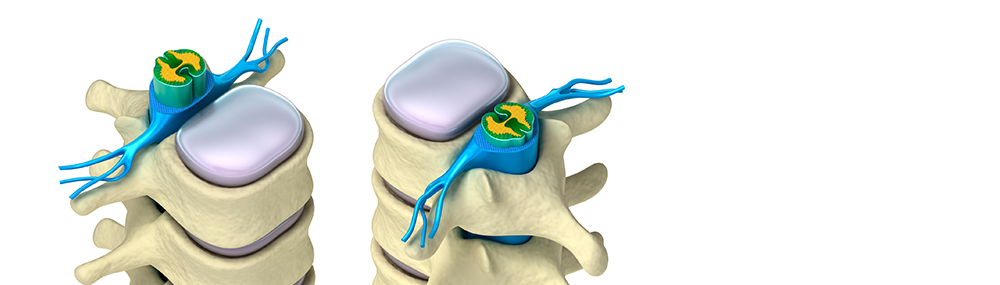
Spinal stenosis is a narrowing of the spinal canal, which places pressure on the spinal cord. It may be in the neck or the lower back. While spinal stenosis can be found in any part of the spine, the lumbar and cervical areas are the most commonly affected.
What causes it?
Some patients are born with this narrowing, but most often spinal stenosis is seen in middle aged patients. Stenosis is the gradual result of aging and “wear and tear” on the spine during everyday activities. There may be a genetic predisposition to this since only a minority of individuals develops advanced symptomatic changes. As you get older, the ligaments of the spine can thicken and harden (calcification). Bones and joints may also enlarge, and bone spurs (osteophytes) may form. Bulging or herniated discs are also common. Spondylolisthesis (slipping of one vertebra on another) also occurs and leads to compression. When these conditions occur in the spinal area, they can cause the spinal canal to narrow, creating pressure on the spinal nerve.
What symptoms does it cause?
When inflammation of the nerves occurs at the level of increased pressure problems may start. Patients with lumbar spinal stenosis may feel pain, weakness, or numbness in the legs, calves or buttocks. In the lumbar spine, symptoms often increase when walking short distances and decrease when you sit, bend forward or lie down. Cervical spinal stenosis may cause similar symptoms in the shoulders, arms, and legs; hand clumsiness and gait and balance disturbances can also occur. In some patients the pain starts in the legs and moves upward to the buttocks; in other patients the pain begins higher in the body and moves downward. The pain may radiate like sciatica or may be a cramping pain. In severe cases, the pain can be constant. Severe cases of stenosis can also cause bladder and bowel problems. Paraplegia or significant loss of function is rare.
How it is diagnosed?
Before making a diagnosis of stenosis, it is important for Dr.Rao to check your:
- History: Dr.Rao will begin by asking you to describe any symptoms are having and how the symptoms have changed over time. Dr.Rao will also need to know how you have been treating these symptoms including what medications you have tried.
- Physical Examination: Dr.Rao will then examine you by checking for any limitations of movement, problems with balance and signs of pain. Dr.Rao will also look for loss of extremity reflexes, muscle weakness, sensory loss, or abnormal reflexes which may suggest spinal cord involvement.
- Tests: After examining you, Dr.Rao can use a variety of tests to look at the inside of the body. Examples of these tests include:
- X-rays – these tests can show the structure of the vertebrae and the outlines of joints and can detect calcification.
- MRI (magnetic resonance imaging) – this test gives a three-dimensional view of parts of the back and can show the spinal cord, nerve roots, and surrounding spaces, as well as enlargement, degeneration, tumors or infection.
- Computerized axial tomography (CAT scan) – this test shows the shape and size of the spinal canal, its contents and structures surrounding it. It shows bone better than nerve tissue.
- Myelogram – a liquid dye is injected into the spinal column and appears white against bone on an x-ray film. A myelogram can show pressure on the spinal cord or nerves from herniated discs, bone spurs or tumors.
- Bone scan – This test uses injected radioactive material that attaches itself to bone. A bone scan can detect fractures, tumors, infections, and arthritis, but may not tell one disorder from another. A bone scan is usually performed along with other tests.
Non-surgical Treatment of Stenosis
There are a number of ways a doctor can treat stenosis without surgery. These include:
- Medications, including non-steroidal anti-inflammatory drugs (NSAIDs) to reduce swelling and pain, and analgesics to relieve pain.
- Corticosteroid injections (epidural steroids) can help reduce swelling and treat acute pain that radiates to the hips or down the leg. This pain relief may only be temporary and patients are usually not advised to get more than 3 injections per 6-month period.
- Rest or restricted activity (this may vary depending on extent of nerve involvement).
- Physical therapy and/or prescribed exercises to help stabilize the spine, build endurance and increase flexibility.
When should you consider surgery?
If you have tried all the treatment options that you feel are reasonable, if your pain is intolerable, if you feel your function is not acceptable, if you are getting worse despite whatever you try, if your weakness is no longer something tolerable, if you are concerned that your weakness may become permanent, certainly consider surgery as a good option. If you are developing numbness in your private areas, or if you are having accidents with your urine or stool function, please talk to Dr.Rao immediately. Surgery may be necessary right away to avoid permanent nerve damage.
Surgical Treatment of Stenosis
In many cases, non-surgical treatments do not treat the conditions that cause spinal stenosis, however they might temporarily relieve pain. Severe cases of stenosis often require surgery. The goal of the surgery is to relieve pressure on the spinal cord or spinal nerve by widening the spinal canal. This is done by removing, trimming, or realigning involved parts that are contributing to the pressure.
The most common surgery in the lumbar spine is called decompressive laminectomy in which the lamina (roof) of the vertebrae are removed to create more space for the nerves. Dr.Rao may perform a laminectomy with or without fusing vertebrae or removing part of a disc. Various devices (like screws or rods) may be used to enhance fusion and support unstable areas of the spine.
Other types of surgery to treat stenosis include the following:
- Laminotomy – when only a small portion of the lamina is removed to relieve pressure on the nerve roots;
- Foraminotomy – when the foramen (the area where the nerve roots exit the spinal canal) is removed to increase space over a nerve canal. This surgery can be done alone or along with a laminotomy;
- Medial Facetectomy – when part of the facet (a bony structure in the spinal canal) is removed to increase the space;
- Anterior Cervical Discectomy and Fusion – the cervical spine is reached through a small incision in the front of the neck. The intervertebral disc is removed and replaced with a small plug of bone, which in time will fuse the vertebrae.
- Cervical Corpectomy – when a portion of the vertebra and adjacent discs are removed for decompression of the cervical spinal cord and spinal nerves. A bone graft, and in some cases a metal plate and screws, is used for stability.
- Laminoplasty – a posterior approach in which the cervical spine is reached from the back of the neck and involves the surgical reconstruction of the posterior elements of the cervical spine to make more room for the spinal canal.
- Coflex – The coflex® Interlaminar StabilizationTM device is a new, non-fusion solution that can provide spinal stability — with greater mobility and faster recovery* — than spinal fusion surgery.