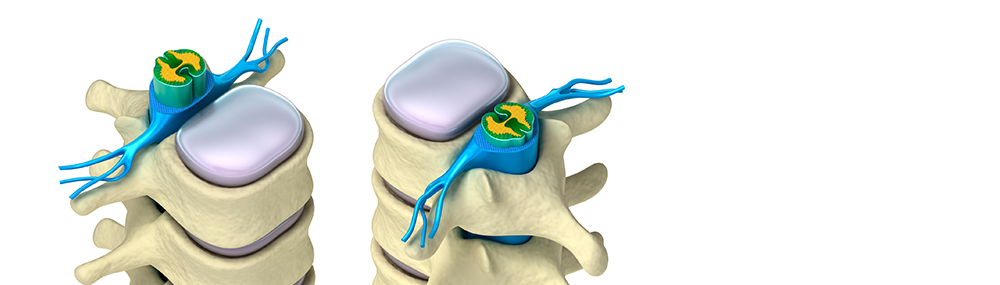
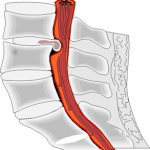
 Herniated discs are a common source of lower back pain. Discs are cushions found between the vertebrae that make up the spinal column. In the middle of the spinal column is the spinal canal that contains the spinal cord and other nerve roots. The discs between the vertebrae allow the back to flex or bend. Discs also act as shock absorbers. The outer edge of the disc is a ring of cartilage called the annulus. The center of the disc is a gel-like substance called the nucleus. A disc herniates or ruptures when part of the center nucleus pushes the outer edge of the disc into the spinal canal, and puts pressure on the nerves.
Herniated discs are a common source of lower back pain. Discs are cushions found between the vertebrae that make up the spinal column. In the middle of the spinal column is the spinal canal that contains the spinal cord and other nerve roots. The discs between the vertebrae allow the back to flex or bend. Discs also act as shock absorbers. The outer edge of the disc is a ring of cartilage called the annulus. The center of the disc is a gel-like substance called the nucleus. A disc herniates or ruptures when part of the center nucleus pushes the outer edge of the disc into the spinal canal, and puts pressure on the nerves.
As people age, the water content of the disc decreases, so it begins to shrink and the spaces between the vertebrae get narrower. Also, the disc itself becomes less flexible. Other conditions that can weaken the disc include:
- wear-and-tear
- excessive weight which can squeeze the softer material of the nucleus out toward the spinal canal
- bad posture
- improper lifting
- sudden pressure (which may be slight)
The fibrous outer ring may tear. As the disc material pinches and puts pressure on the nerve roots, pain results. Sometimes fragments of the disc enter the spinal canal where they can damage the nerves that control bowel and urinary functions.
Recognizing symptoms
Low back pain affects four out of five people. So pain alone isn’t enough to recognize a herniated disc. However, if the back pain is the result of a fall or a blow to your back, don’t hesitate to contact an orthopedic doctor. The most common symptom of a herniated disc is sciatica, a sharp, often shooting pain that extends from the buttocks down the back of one leg. This is caused by pressure on the spinal nerve. Other symptoms include:
- Weakness in one leg
- Tingling (a “pins-and-needles” sensation) or numbness in one leg
- Loss of bladder or bowel control (If you also have weakness in both legs, you could have a serious problem. Seek immediate attention.)
- A burning pain centered in the back
In disc herniations, the L5-S1 disc is involved 45% to 50% of the time, L4-5 40% to 45%, and L3-4 about 5%. Disc herniation at the other lumbar levels is rare. Sometimes the herniation is lateral, i.e., into the foramen. This is known as a far lateral disc herniation and occurs in about 3% to 10% of cases. Symptoms and signs vary, and it is common for different combinations of muscle and sensory loss to be present.
Diagnosing a herniated disk
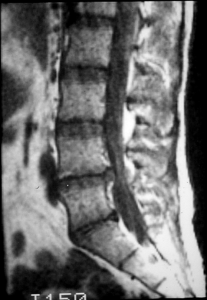
Your medical history is key to a proper diagnosis. You may have a history of back pain with gradually increasing leg pain. Often a specific injury causes a disc to herniate. A physical examination by an orthopedic specialist like Dr. Rao can usually determine which nerve roots are affected (and how seriously). A simple x-ray may show evidence of disc or degenerative spine changes. MRI or CT scans or an EMG (nerve test) may be recommended if pain continues.
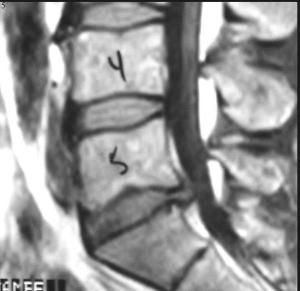
On the left image see the disc protruding below (disc #5), pushing the nerve sac to your right.
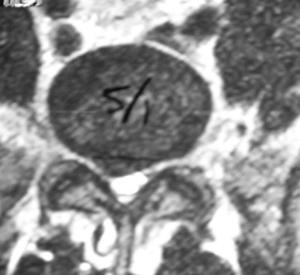
On the right image, you will see the dark gray disc material pushing the nerve sac down at the 5-1 level.
| Disc Level | Root Comp | Weakness | Reflex Involvement | Sensory Loss | Pain Distribution |
|---|---|---|---|---|---|
| L3 – L4 | L4 | Quadriceps, tibialis anterior | Knee jerk | Medial knee and shin | Anterior thigh |
| L4 – L5 | L5 | Extension of big toe | No significant | Big toe | Back of thigh, lateral calf |
| L5 – S1 | S1 | Gastrocnemius (ankle plantar flexion) | Achilles | Lateral foot and heel | Back of thigh and calf |
Treatment options
Non-surgical treatment from an orthopedic specialist usually works. Most back pain will resolve gradually with simple measures. Bed rest and over-the-counter pain relievers may be all that’s needed. Muscle relaxers, analgesic and anti-inflammatory medications are also helpful. You can also apply cold compresses or ice for no more than 20 minutes at a time, every hour or several times a day as necessary. After any spasms settle, you can switch to gentle heat applications.
Any physical activity should be slow and controlled so that symptoms do not return. Take short walks and avoid sitting for long periods. Exercises may also be helpful in strengthening back and abdominal muscles. Learning to stand, sit, and lift properly is essential to avoiding future episodes of pain.
Other treatments
- If non-surgical treatment fails, epidural injections of a cortisone-line drug may lessen nerve irritation and allow better participation in physical therapy. These shots are given on an outpatient basis over a period of weeks.
- Surgery may be required if a disc fragment lodges in spinal canal and presses on a nerve, causing a loss of function. The traditional surgical treatment is called a laminectomy and involves removing a portion of the vertebral bone. The surgery is performed under general anesthesia with an overnight hospital stay.
- Newer surgical techniques are microscopic and minimally invasive. Surgery is performed on an outpatient basis and you should be able to return to work in a few weeks.